Varicose veins of the lower extremities is a disease characterized by impaired functioning of the veins in the legs.It can occur without visible signs or have a clear venous pattern - it all depends on the type and stage.An integral component of this disease is the disruption of the venous valves, without which the vein ceases to function properly.This leads to the appearance of dilated veins and poor circulation in the leg.
Causes of varicose veins
Venous blood moves upward, from the toes to the torso; if the process is disrupted, then it lingers in the legs.The heart cannot create enough suction force to lift the blood upward.There are a number of mechanisms, the main one of which is the muscle pump (muscular-venous pump).Valves set the direction of blood flow - causing it to move from bottom to top.If, under the force of gravity, the blood tries to return back, the valves will close and will not let it through.
During contraction of the leg muscles, for example during walking, the blood in the vein is “squeezed out” and directed towards the body.During muscle relaxation, the vein fills with blood, which is “sucked” from below.Failure of the mechanism leads to varicose veins of the lower extremities.
There are several factors that provoke the onset of the disease.They are divided into 2 large groups:
- Hereditary.One of the parents or close relatives has the pathology.This is the cause of varicose veins in 90% of patients.
- Acquired.Occurs due to the adverse effects of provoking factors.
The main culprit is genetics.And additional circumstances are already imposed on it:
- a profession that involves standing or sitting for a long time (salespeople, office workers, drivers, surgeons);
- pregnancy as a “hormonal revolution” in a woman’s body (veins stretch and become noticeable, after childbirth they are not always restored and with each new pregnancy the situation worsens);
- diseases of the pelvic organs impede outflow and increase pressure in the veins;
- taking hormonal drugs (make vascular walls less elastic);
- excessive passion for warming procedures (visiting a bathhouse, sauna);
- increased intra-abdominal pressure (with chronic cough or constipation);
- heavy physical work, carrying heavy loads (loaders, dockers, builders);
- excess body weight (more blood volume means more load on the vessels);
- injuries affecting veins and impairing blood circulation;
- biological factors - old age, high growth;
- bad habits (alcohol, cigarettes)
- lack of physical activity;
- wearing compressive clothing.
The veins rest when a person lies down, and the blood practically flows through them in the direction from the legs to the heart.They enjoy working when their muscles actively help them while walking.Veins experience enormous stress when a person stands or sits.Whether they can withstand this load or not depends on heredity and the presence of other provoking factors.
Now that we’ve figured out the reasons, let’s move on to the symptoms of varicose veins.
How does varicose veins manifest?
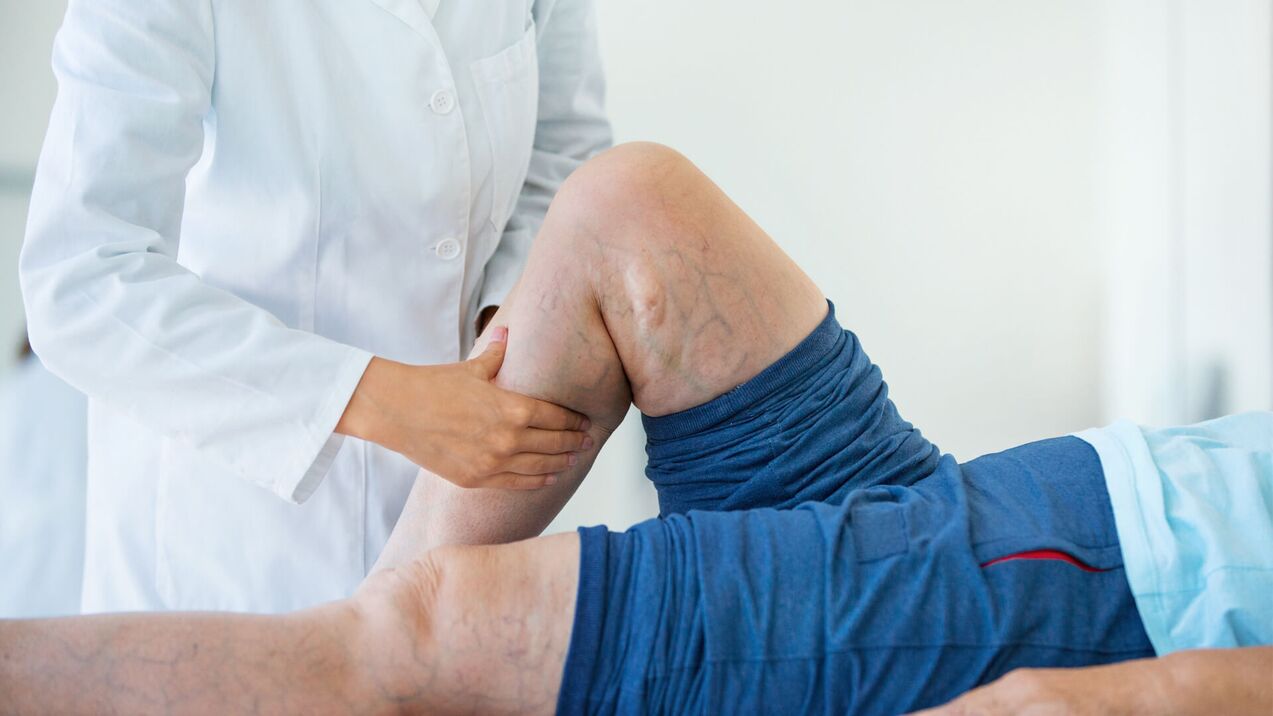
Symptoms of varicose veins in women and men are generally similar, although they have slight differences
The most obvious symptom is the presencedilated veins of the lower extremitiesdifferent sizes:
- Up to 1 mm – telangiectasia or spider veins;
- from 1 to 3 mm – reticular (tortuous);
- from 3 mm – varicose veins.
Insufficient functioning of the muscular-venous pump is expressed by swelling of the legs.It begins in the lower third of the leg and rises to the level of the knee joint.
If the legs are in a vertical position for a long time without moving, then the blood stagnates, and its liquid part “sweats” through the wall of the vessel into the surrounding tissues.Swelling forms.When lying down, the limbs do not swell, becausecirculation occurs naturally and easily.
How can you tell if there is swelling?Look at the location of the sock elastic.After removal, a trace remains, which means the liquid is poorly removed and accumulates in the tissues.
Symptoms of edema with varicose veins:
- occur towards the middle of the day;
- worsens in the evening due to prolonged standing or sitting;
- pass overnight while a person sleeps;
- do not move to the foot.
Venous edema in the legs is usually accompanied byfeeling of heaviness, which can be perceived as “tension” or “humming” in the calf muscles or throughout the lower leg.
Can often be bothersomenight cramps of the lower extremities.The reason for this is the retention of venous blood, which disrupts the metabolic processes occurring in the muscles.This causes severe spasm of the calf muscles, usually triggered by stretching during sleep.The leg seems to be severely cramping, which is why the person wakes up.
Dry skin on legsis a consequence of tissue nutritional disturbances.Toxins that are not removed through the bloodstream disrupt the normal functioning of cells.The epidermis becomes less elastic and loses moisture, which leads to flaking.
Long-term venous insufficiency increases vascular permeability.The liquid part and formed elements of the blood “sweat” through the wall into the surrounding tissue, where they are destroyed.Blood pigments spread under the skin - outwardly it looks likehyperpigmentation, darkening of the epidermis with the formation of brown spots.
The process is often accompaniedtissue compaction(induration), which occurs due to deterioration of blood supply and insufficient nutrition for a long time.At the same time, the structure of the skin and subcutaneous tissue is rebuilt, they become more connective fibers and less elastic.Most often, this phenomenon is observed on the lower third of the lower leg on the inside.
If the disease is not treated, it will get worse.In the later stages, trophic ulcers appear.A long-term non-healing wound is located on the inner surface of the lower third of the leg.It can be the size of a five-kopeck coin or encircle the entire shin.
Complications of varicose veins
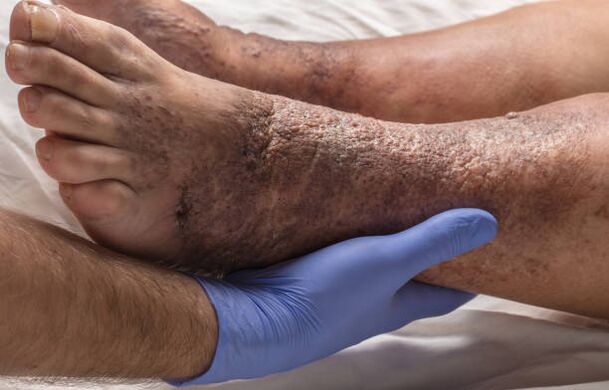
Inflammation of the saphenous veins, the formation of blood clots and their separation, blockage of the pulmonary arteries, skin changes, trophic ulcers - all these are complications of varicose veins, the consequences of a long-term pathology.
Thrombophlebitis- inflammation of the saphenous veins.A blood clot forms in the superficial vessels, which is accompanied by an inflammatory reaction.A dangerous condition that threatens to spread into deeper veins.Part of the clot can break off and travel through the heart to the lungs, blocking a pulmonary artery.This condition is called pulmonary embolism (PE).
Thrombophlebitis is usually treated on an outpatient basis, but treatment methods depend on the patient’s condition and many associated factors and are prescribed by a doctor.
Phlebothrombosis– formation of blood clots in deep veins.The complication leads to constant swelling and pain, fraught with separation of part of the blood clot and the development of pulmonary embolism.Treatment of phlebothrombosis takes place in a hospital, with hospitalization.
PE (pulmonary embolism)– a condition in which a blood clot breaks off and travels to the pulmonary artery.With thromboembolism, there is a risk of sudden death, when a blood clot clogs an artery and causes suffocation, chest pain, and pulmonary infarction.
Blockage of the small branches of the pulmonary artery may be asymptomatic, but have serious consequences.Massive pulmonary embolism is treated exclusively in intensive care.
Chronic venous insufficiency (CVI)- the result of a delay in venous blood flow in the legs due to a “breakdown” of the valve mechanism.
I will describe it schematically this way: the human body consists of cells that need to be fed.To do this, fresh, oxygen-rich and nutrient-rich arterial blood reaches all cells and tissues.After the cells “eat”, they form “waste”, which is dumped into the veins.Venous blood is purified, saturated with oxygen and converted into arterial blood.The circle closes.
What happens in case of circulatory problems?Outflow is delayed and waste is not removed.Tissues begin to suffer and turn from normal to bad (sick).All processes change.The vascular walls leak fluid, forming edema.Pain occurs.Over time, the intercellular space changes, the subcutaneous tissue becomes coarser and “shrinks,” the skin darkens and thickens, and long-term non-healing ulcers appear.
Hyperpigmentation and lipodermatosclerosis– consequences of chronic VN.These are not life-threatening conditions, but they do impair quality of life.The feeling of skin tension and its unaesthetic appearance causes discomfort.Complications decrease after treatment of varicose veins.
Varicose eczema– inflammation of the skin of the lower leg with redness and itching, weeping areas and peeling.Outwardly it resembles ordinary eczema, only it is treated differently: without eliminating the underlying disease (venous insufficiency), any ointments will be ineffective.
Trophic ulcer– an open wound that does not heal for more than 2 months.Occurs due to impaired tissue nutrition.Poor blood flow and stagnation limit the supply of nutrients to cells, which prevents them from multiplying normally and filling the skin defect with new structures.It is pointless to treat ulcers with ointments alone; an integrated approach is needed using several methods to eliminate CVI.
Bleeding from varicose veinscan occur even with minor injuries in the shin area and is often severe, becausein dilated vessels, blood pressure is higher than normal.Stopping bleeding is easy: apply a sterile cloth to the wound and bandage it tightly.Do not use a tourniquet; if the limb is numb or tingling, loosen the bandage.Additionally, raise your leg higher.
Diagnostics
Making a diagnosis begins with a consultation.The doctor finds out whether the problem is really varicose veins and only that.In my practice, there were cases with symptoms of varicose veins, but they had nothing to do with it.Edema is caused by heart failure, lymphedema, and allergies.
The clinical picture may not indicate varicose veins, but another disease.Pain in the calf muscles is associated with atherosclerosis of the arteries, osteochondrosis, and flat feet.The causes of trophic ulcers are hypertension, skin infection, stroke and damage to peripheral nerves.
A phlebologist will conduct a differential diagnosis and make an accurate diagnosis, find out what is causing your symptoms.A reliable diagnostic method is duplex study.It helps to clarify the condition of blood vessels and develop individual patient management tactics.
Computed tomography, MRI venography, and venography are rarely used today.
How to treat?
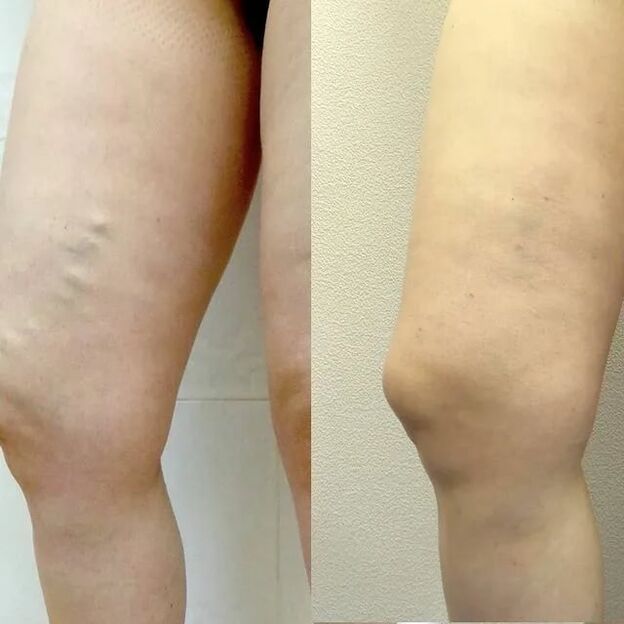
Treatment should always be comprehensive.The doctor has three directions at his disposal:
First -compression elastic knitwear.This includes knee socks, stockings and tights.They all have different degrees of pressure.The type of knitwear and the degree of compression are selected individually depending on the nature and stage of the pathology.
I would like to note: if you have tried wearing compression garments, but have not noticed any improvement or your condition has worsened, then you need to consult a doctor.You may have a disease other than varicose veins; the products may be of poor quality or used incorrectly.It is necessary to find out why there is no positive dynamics.
Second -drug therapy.The range of drugs that reduce the manifestations of CVI is large.Some medications are stronger, some are weaker.The doctor selects the drugs, taking into account the manufacturer, dosage, regimen and duration.
Third -surgery.There are several types of operations: phlebectomy (removal of dilated veins through incisions), miniphlebectomy (removal through punctures), laser obliteration (laser sealing), radiofrequency ablation (heat sealing).Each method has its own advantages and disadvantages, opportunities and limitations.The phlebologist decides which method or combination of methods is right for you.
























